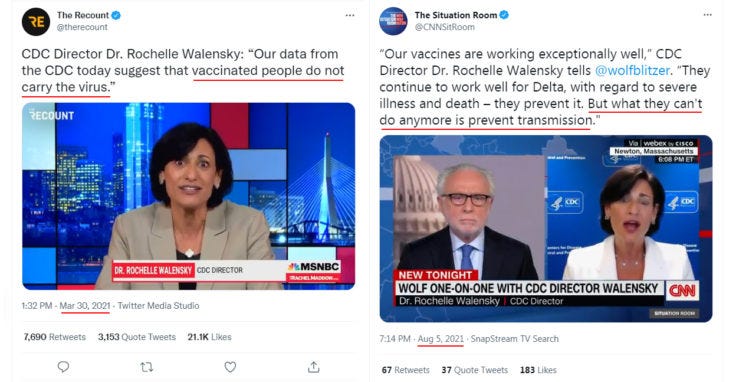
Note: This is all evidence from prior to Omicron. However, this article provides evidence that even when the Alpha and Delta variants were dominant and the vaccines were so called “more” effective, vaccine mandates still weren’t supported by the evidence. A separate article on vaccine mandates during the Omicron dynasty is coming soon.
Vaccine Effectiveness Against Symptomatic Cases
At the start of vaccination campaigns around the world, official country data showed that the vaccines were effective at reducing hospitalizations and deaths in at-risk demographics, matching the primary outcome measures of the vaccine clinical trials. Official tracking data by country also appeared to show a decline in cases (symptomatic) which lends support to the suggestion that mass COVID-19 vaccination would also reduce transmission rates in the population; less symptomatic cases should equal fewer chances for transmission. However, as time passed from the start of mass vaccination a different picture emerged.
Most recent data suggest that the COVID-19 vaccines are still somewhat protective against hospitalization and death, specifically from COVID-19; however, their effectiveness against symptomatic cases and asymptomatic infections wanes quickly and significantly. A report from Israel’s Ministry of Health in early July 2021 reported that vaccine effectiveness against infection had dropped to 39% (CI 9%-59%) (1). Recent studies have also confirmed the observations noted by Israel. COVID-19 vaccine effectiveness decreases to approximately 50% by as early as 3-4 months following full vaccination and to statistically zero by 5-6 months following vaccination (2, 3, 4, 5, 6). To put this into perspective, early in the pandemic, the United States FDA listed a minimum effectiveness of 50% for any COVID-19 vaccine to be considered for emergency authorized use (7). Therefore, the evidence suggests that, as early as 3 months after complete vaccination, the current COVID-19 vaccines no longer meet the minimum required level of efficacy for emergency authorized use.
Such significant decreases in COVID-19 protection against SARS-CoV-2 infection is further supported by drastically reduced neutralizing antibody levels within months of vaccination (8). Levin et al. compare this rapid reduction in SARS-CoV-2 neutralizing antibodies over a few months with neutralizing antibody levels from other common vaccines where only a 5-10% per year reduction in neutralizing antibody levels is seen (8).
Effectiveness Against Emerging Variants
Not only does COVID-19 vaccine efficacy against symptomatic cases wane quickly, they are also less effective against emerging variants. A growing body of evidence shows that SARS-CoV-2 variants such as the currently dominant Delta, along with the Lambda and Gamma variants are more resistant to vaccine-based immunity in comparison to wild type SARS-CoV-2 and the Alpha variant (9, 10, 11, 12, 13, 14, 15). Additionally, genetic studies suggest that continued mutations in SARS-CoV-2 spike protein may create variants that fully evade current COVID-19 vaccine-based antibodies (16). Variant A.30 provides real-world evidence of this theory (17). Note: Omicron is now also a real world example of this.
Effectiveness Against Asymptomatic Infection
As outlined, a large body of evidence supports the rapid waning of COVID-19 protection against symptomatic cases and reduced protection against emerging variants. However, this evidence also shows that protection against asymptomatic infection is even weaker. At peak timing of vaccine effectiveness, protection against asymptomatic infection may only reach 44% to 63.7% (3, 18). By 5 weeks following full vaccination, effectiveness against asymptomatic infection decreases to approximately 50%, by week 10 effectiveness decreases to 38.5%, and by week 15 effectiveness decreases to statistically zero (3). Additionally, seroconversion evidence suggests that asymptomatic infection in the vaccinated occurs frequently (19).
Transmission from Asymptomatic Breakthrough Infections
At first glance, since the evidence outlined in my previous article shows that unvaccinated asymptomatic transmission is not a main driver of the COVID-19 pandemic, asymptomatic breakthrough infections should not be concerning.
However, recent evidence shows that asymptomatic and presymptomatic vaccine breakthrough infections can carry a higher viral load than asymptomatic unvaccinated infections (13, 14, 20, 21). Furthermore, evidence from Vietnam shows that vaccinated infections carry viral loads up to 251 times higher than viral loads measured before the start of vaccination (22).
Although viral loads in asymptomatic infection are not proof of asymptomatic transmission, emerging evidence continues to show that transmission is occurring from asymptomatic/presymptomatic breakthrough infections (20, 22, 23). Since vaccination reduces the severity of symptoms, it is likely to reduce the chance that someone with a breakthrough infection will get tested. Therefore, since vaccination does not prevent viable viral replication in the mucosal membrane, prevents the severity of systemic symptoms, and reduces the chance of being tested, it is suggested that the transmissibility of asymptomatic breakthrough infections may be underestimated by a factor of 2 (21). Additionally, new evidence shows that the risk of household transmission from the vaccinated to the vaccinated is higher than from the vaccinated to the unvaccinated (15).
Transmission from Symptomatic Breakthrough Cases
Aside from asymptomatic/presymptomatic breakthrough transmission, evidence shows that transmission from symptomatic breakthrough cases is also common. Viral loads in unvaccinated and breakthrough cases are consistently shown to be equal, and breakthrough case transmission is clearly being demonstrated in contact tracing studies (Ref, 13, 14, 15, 21, 22, 24, 25, 26, 27, 28, 29, 30). At best, there was a 45-50% reduction in transmission from the vaccinated compared to the unvaccinated; however, much of this evidence comes from vaccinees during the peak timing of vaccine effectiveness (full vaccination occurred within 3 months of the study) and not during periods of Delta variant dominance (21, 31, 32). Evidence from other studies, particularly during Delta variant dominance, shows that there is little to no difference between transmissibility from vaccinated or unvaccinated symptomatic cases (14, 21, 24, 25).
Vaccination Population Coverage and COVID-19 Cases
The scientific literature provides evidence that the effectiveness of the COVID-19 vaccines wane quickly, they are not effective against new variants, they do not significantly reduce SARS-CoV-2 transmission, and may even enhance transmission. This evidence is also being seen in real-world data.
Data from the weekly government COVID-19 surveillance reports out of the United Kingdom show that the case incidence per 100,000 people is higher in the vaccinated population for all age groups above age 29 years than it is for the unvaccinated (33). Note: This trend has become more pronounced as of the date of writing of this substack article.
In a peer-review paper published in September 2021, Subramanian and Kumar analyzed the data from OurWorldInData.org to determine the relationship between population vaccination coverage and COVID-19 cases per million people (34). Of the 68 countries with fully reported vaccination data, no relationship between the percentage of population vaccinated and COVID-19 case rate per million people was found. The authors further suggested that there is a marginally positive association such that the higher the percentage vaccinated, the higher the COVID-19 case rate per million people is. As an example, Israel had over 60% of their population fully vaccinated at the time and they had by far the highest case rate. Further perspective can be gained through data from Iceland and Portugal who, at the time, had over 70% of their populations fully vaccinated yet had higher COVID-19 cases per million than Vietnam and South Africa who only had 10% of their populations vaccinated.
Subramanian and Kumar also made this comparison between United States counties from data obtained through the White House COVID-19 Team (34). Complete vaccination data were available for 2947 counties. The author’s comparison yielded the same findings as the country comparison, no relationship between the percentage of population vaccinated and COVID-19 case rate per 100,000 people was found. Furthermore, out of the 5 counties with the highest percentage of population vaccinated at that time, 4 of them were listed as high transmission counties by the CDC. Additionally, 15 out of the 57 counties (26%) listed by the CDC as low transmission counties, had less than 20 percent of their populations vaccinated. Note: A recent pre-print study from November 2021 reviewed data from 145 countries and found that vaccination population coverage was related to an increase in COVID-19 cases and also an increase in the rate of death (35).
The evidence that vaccine effectiveness wanes very quickly; is less effective against emerging variants; does not reduce transmission from symptomatic breakthrough cases; allows for transmission from asymptomatic/presymptomatic breakthrough infections, which is rare in unvaccinated infections; and COVID-19 case numbers are not associated with the percentage of the population vaccinated suggests that the unvaccinated population does not pose a greater risk of SARS-CoV-2 transmission than the vaccinated. Furthermore, the vaccine passports/mandates convey the impression that the vaccinated are not at risk of transmitting to others, leading to increased behaviors in the vaccinated population that promote ongoing transmission, including socializing in close quarters with mild to moderate symptoms. Thus, the presented evidence challenges the popular narrative that the pandemic is now one of the unvaccinated, it may possibly be one of the vaccinated. Regardless, it is inherently wrong to vilify either of these groups of people as history shows that discrimination and segregation of groups of people is dangerous to our humanity (36).
Vaccination Coverage and The Law of Diminishing Returns
Aside from the serious concerns about vaccine efficacy and the fact that they do not significantly reduce transmission for a substantial period, the law of diminishing returns should also be considered. From an economics standpoint, this theory predicts that beyond a certain point, additional inputs produce smaller and smaller outputs. This theory is also applied to clinical medicine and has been explained as follows: “For example, when the risk of an adverse event can be reduced in several different ways, the impact of each intervention can generally be shown mathematically to be reduced by the previous ones. The diminishing value of successive interventions is further reduced by adverse consequences (eg, drug-drug, drug-disease, and drug-nutrient interactions), as well as by the total expenditures of time, energy, and resources, which increase with each additional intervention.” (37).
Applied to the necessity for vaccine passports/mandates, the COVID-19 vaccines are the input/intervention, and COVID-19 cases and infections are the output/adverse event. Therefore, if many countries have had almost all the elderly and other high-risk populations fully vaccinated, along with 65% or more of the remaining population, and the pandemic continues, having the remainder of the population vaccinated cannot be considered the solution as the return from each increasing percentage of the population vaccinated will continue to diminish in its impact on case/infection numbers. This law would still apply even in a best-case scenario where the vaccines do not suffer from the numerous flaws outlined above.
Vaccine Mandates and Passports Don’t Make Sense
I am against vaccine mandates on principal. However, for argument sake, in order to scientifically prove the necessity of COVID-19 vaccine mandates/passports that violate understood basic human rights, several criteria would need to be satisfied with exceptional, indisputable scientific evidence:
A significant threat must be present for a large portion of the population.
Transmission from unvaccinated, asymptomatic infections must be a significant driver of the pandemic.
There are no other effective, safe treatments available.
The vaccine must be safe beyond any reasonable doubt.
The vaccine must significantly reduce transmission from asymptomatic infections and symptomatic cases.
If there is significant doubt about any 1 of these outlined criteria it would be sufficient to conclude that vaccine mandate/passport policies should not move forward.
I cast significant doubt on number 1 here:
and number 2 here:
And finally, this current article casts significant doubt on number 5.
Therefore, upon review of the scientific literature, exceptional, indisputable evidence does not exist in support of 3 of the 5 outlined criteria. Specifically, a threat significantly greater than seasonal influenza is not present for much of the population, asymptomatic/presymptomatic transmission from the unvaccinated is not a significant driver of the pandemic, the vaccines do not significantly reduce transmission from breakthrough cases, the vaccines allow for transmission from asymptomatic breakthrough infections, and vaccine population coverage percent is not associated with reduced COVID-19 cases. Therefore, since the current evidence does not support three out of the five outlined criteria, it is concluded that vaccine passport/mandate policies are unnecessary and ineffective.
NOTE: The arrival of Omicron and the data gathered since then has simply strengthened the argument against the vaccine mandates/passports: Omicron is less deadly, more transmissible, avoids vaccine immunity, shows equal transmissibility in the vaccinated and nonvaccinated, and country data shows infectivity rates are higher for the vaccinated population. I will be writing an article on this shortly.
I did not write about alternative treatments or vaccine safety (points number 3 and 4). If you would like to learn more about those things, check out the following substacks and websites.
Front-Line COVID-19 Critical Care Alliance - COVID-19 treatment information